It is hard to think of a person who doesn’t have at least one scar. In general, scars are permanent “marks” on the skin resulting from an injury. They are formed over the wounded area as a result of the healing process after a skin burn, cut, inflammation, procedure, acne, trauma, etc.
Damage to the deeper layer of the skin – the dermis – is usually a prerequisite for the formation of a scar, whereas the response to the epidermis does not always result in a similar skin issue.
There are different types of scars – acne scars, contractile (affecting the movement of a joint), hypertrophic, stretch marks, and one type that inherently differs radically from the others – keloid scars.
Keloids are types of scars that never stop growing, creating firm, rubbery nodules in the area, where the skin got injured.
The expanded and damaged connective tissue is characterized by a raised edge, irregular shape and excessive collagen deposition, usually as a result of impaired skin integrity. The most visible keloids are formed after severe skin burns.
Keloids are tumor growths of connective tissue over the skin level. They are in the form of a hypertrophic rupture that extends beyond the site of the injury itself. The process of keloid scar formation slows down after a particular period of time and, unfortunately, can lead to significant cosmetic defects.
Keloids are an individual reaction to the damaged skin and may result in the appearance of multiple blood vessels. The scar tissue that doesn’t stop growing is much larger than the wound causing the scar.
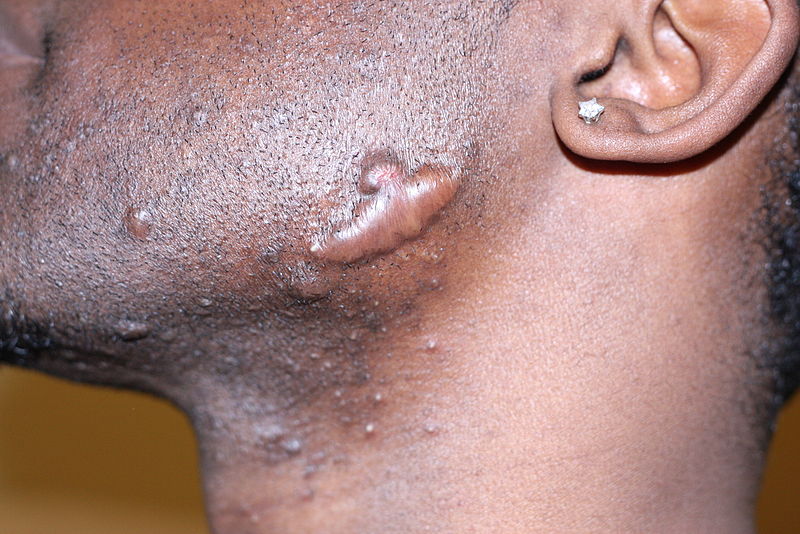
Keloids look like benign tumor tissue around the site of the injury and rise over the normal skin. They are smooth to the touch and have pink or purple color.
Unlike other types of scars, keloids do not diminish over time, but may even increase in size, while their color may get darker and even more noticeable.
Although keloid scars often cause itching, they are usually not a threat to your skincare. They may cause discomfort or irritation when clothes cover them or there are other forms of contact or friction available.
Rarely, their appearance spreads over large parts of the body, and this could limit some of the body movements.
Severe burns, cuts or acne breakouts are the most common reasons leading to keloid scarring, but not every scar leads to the development of a keloid.
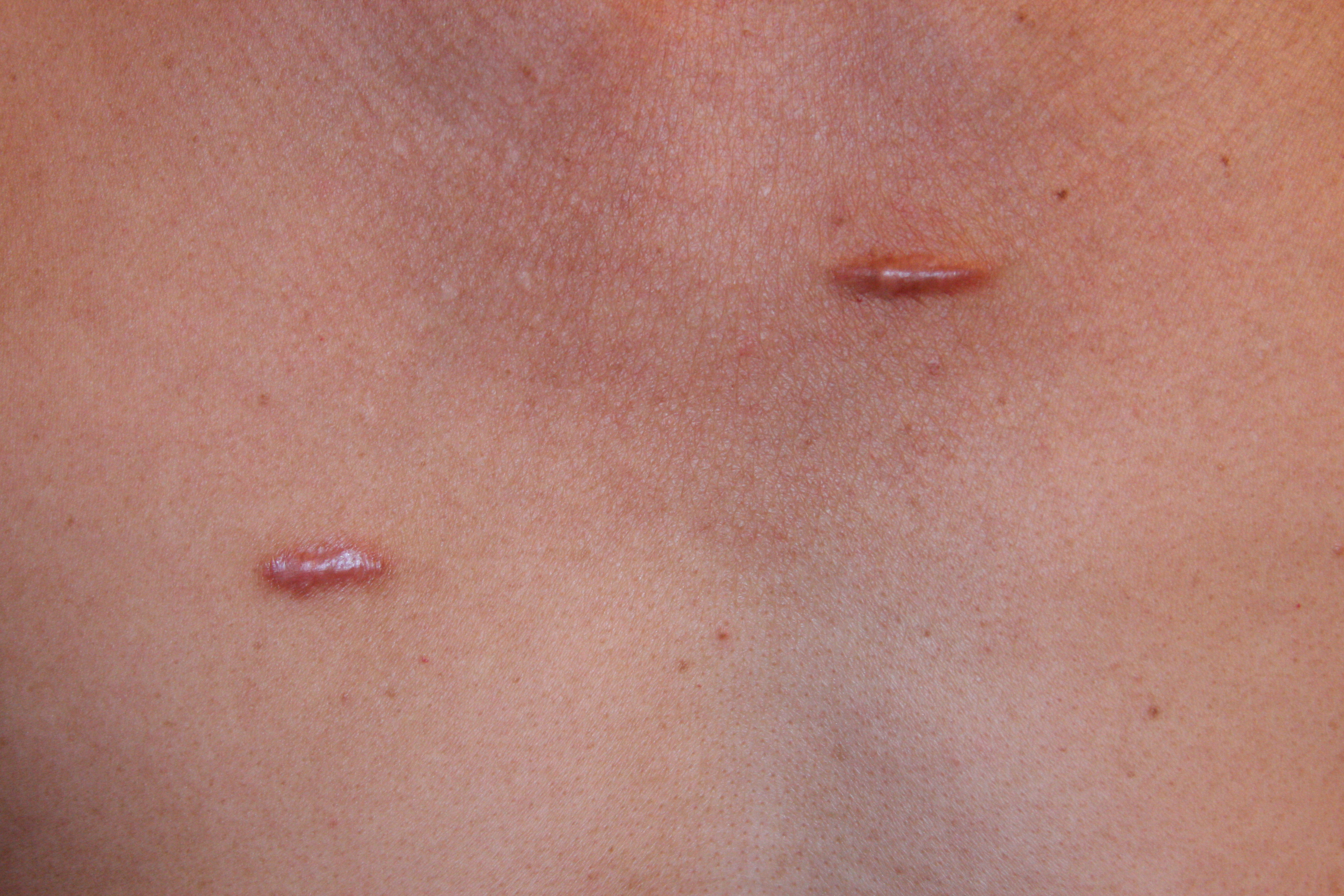
People with darkly pigmented skin are 15 times more likely to develop keloids, and those in the African, Latin and Asian ethnic groups are at greatest risk. This type of scarring is equally common in both men and women, rarely occurring in elderly people and children.
Keloid scars are more of a cosmetic than a health-related issue. If the keloid scar has appeared on a visible part of the body (for example, in the facial area), it may lead to lower self-esteem and pronounced psychological discomfort.
Exposure to sunlight makes the mark appear darker and more protruding than the rest of the skin surrounding it. Because of that, people who have large keloid scars are looking for efficient solutions to their removal.
There are several ways to eliminate or, at least reduce the appearance of keloid scars:
- Corticosteroid injections (intralesional steroids)
They are safe but moderately painful. Intralesional injections are usually prescribed once every four to eight weeks, targeting the keloids and helping to level the convex skin with the surrounding normal skin.
- Surgical Intervention
This method poses risks because the keloid cut can cause the formation of a similar or even larger sized scar. Some surgeons achieve success by injecting steroids or applying compression (using a specialized pressure device) to the site of the wound months after the removal of the keloid.
- Laser:
The impulse laser can be effective in smoothing the keloids and reducing their prominent pink-purple color. This fixing method is estimated generally safe and considerably less painful but several sessions are needed before a satisfactory result is achieved.
- Occlusive Dressings
The most common forms are cosmetic grade Self-adhesive silicone gel sheets and dressings. These are available without a prescription. The goal is minimizing the wound tension, while constantly hydrating and healing the area affected. Scar sheeting method is proven to reduce keloids with pressures of 15 to 45 mmHg. The course of the application should be at least 6 months for a minimum of 23 h/day, as stated by NCBI (read the clinical study, last updated: March 19, 2019).
According to another study:
-34% of all users with keloids had excellent results
-37.5% showed moderate improvement|
-28% of users claim they had slight to no improvements after the application period
The participants in this clinical trial used self-adhesive silicone sheets (worn 24h/day for about a year).
- Cryotherapy
The method of freezing keloids with liquid nitrogen leads to scar soothing, but they often change their color – the damaged skin darkens or becomes lighter compared to the rest of the skin.
- Interferon
Interferons are proteins produced by the immune system of the body, which have the ability to help with coping with viruses, bacteria and other challenges to the body. Studies performed with interferon injections have shown good results in reducing the size of keloid scarring.
Although there is no universal therapy for the removal of keloid scarring, one of the above-mentioned methods can be recommended after a consultation with a specialist in order to reduce the appearance of the keloid scar. The 100% improvement is rarely possible.
Fixing keloid scarring requires patience and persistence. For some, the optimal effect of the method chosen comes within a couple of months, for others – it may take over a year before the scar becomes flatter and the redness disappears.
Consumers should understand that when it comes to scar removal, the timely treatment is crucial – it will make the scar less symptomatic and will limit the development of the keloid.
![Keloid scar fix [Is it a lost cause?]](https://skinpractice.com/wp-content/uploads/2019/04/800px-Keloid.jpg)




